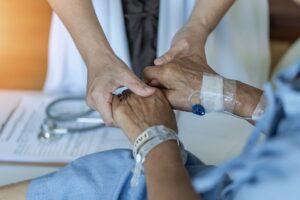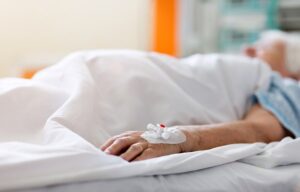
Fortunately, many facilities and caregivers provide above-standard care, but others do not meet our expectations, let alone provide proper care. Many accidents and injuries in nursing care facilities occur because of neglect. Bedsores are a direct consequence of neglect and, if left untreated, can cause severe illness and death.
This guide provides in-depth information about the nature of bedsores, negligent caregiver behaviors that cause them, and steps you can take if your loved one has developed bedsores during their stay at a nursing care facility. We also discuss the physical and financial consequences of bedsores for nursing home residents and those who love them.
Contact an experienced Fort Myers nursing home negligence lawyer from Viles & Beckman, LLC if your loved one has suffered injuries during their stay at a nursing care facility.
What Are Bedsores?
Bedsores refer to damaged skin from sitting or lying in one position for too long. Bedsores have other informal names, too, which include pressure sores, pressure ulcers, or pressure injuries. The formal medical name for a bedsore is a decubitus ulcer. Whether you call them sores or ulcers, bedsores can cause unrepairable skin damage, illness, and excruciating pain for those who develop them.
Bedsores occur because blood flow slows or stops in areas of the body when a person lies or sits in one position too long, creating an open wound. Bedsores typically develop where the skin is closest to the bone. This includes a person’s hips, ankles, heels, back, tailbone, elbows, and shoulder blades. Bedsores can vary in their severity, and medical professionals categorize them based on severity and treatment options. Below is a broad overview of the four stages of a bedsore.
Stage I Bedsores
The genesis of a bedsore is not easy to identify if you do not know the exact signs. A Stage I bedsore subtly changes the skin, but the change is not the same on everyone. Sometimes the area shows some redness and sometimes the skin feels warmer to the touch around the bedsore. You will not notice any breaks in the skin when someone develops a Stage I bedsore.
Stage II Bedsores
Bedsores that have developed into Stage II affect the top layer of the skin formally referred to as the epidermis, and sometimes the layers of the dermis which lie just below the epidermis. A Stage II bedsore can present as a shallow open wound, but it can also look like a big blister that is full of pus. When Stage II bedsores are left untreated, they can break open. This can increase complications associated with the bedsore, especially in terms of cleanliness and lack of proper skincare surrounding the sore.
Stage III Bedsores
A Stage III bedsore is exponentially more serious than Stage I and II bedsores. At Stage III, the bedsore has eaten through most layers of skin and has begun to infect the final layer of skin, primarily made of fat and connective tissues. This layer of skin also houses large nerve endings which means those who suffer Stage III bedsores experience a lot of pain. They can also suffer nerve damage and many more medical issues once the bedsore reaches the final layer of skin. In the most extreme cases of a Stage III bedsore, doctors can see bone and muscle.
Stage IV Bedsores
The most dangerous and painful bedsores occur at Stage IV, where the sore extends into muscle and bone. If you look at a Stage IV bedsore, you can typically see dead skin and a lot of drainage and pus. Those who suffer from the most extreme Stage IV bedsores usually need surgery to remove and reconstruct the area around the bedsore.


Expect More, Receive More: Legal Support That Feels Like Family
Caregiver Neglect Causes Painful Bedsores
Federal and state laws require nursing homes to provide a specific standard of care to those who reside in the facility. Neglect is a criminal act that can result in felony charges when it occurs. Neglect can occur for different reasons. Sometimes nursing care facilities do not have enough nursing assistants, leaving employees overworked. This makes it impossible for caregivers to provide an adequate level of care to all residents no matter how hard they try. Other times, overworked and underpaid nursing assistants are tired and overwhelmed, so they intentionally neglect residents.
Poorly staffed nursing homes put caregivers in situations where it’s easy for them to neglect residents, putting vulnerable residents at risk for bedsores. Residents who are forced to stay in bed without regular repositioning may develop bedsores at some point. The presence of bedsores serves as a strong indicator that caregiver neglect is occurring. So far, we have discussed bedsores in the context of Florida nursing homes, but they can occur in private care settings, too. Those who provide in-home nursing care have the same responsibility to reposition their clients as those who work in nursing homes.
Preventing Bedsores
You cannot directly prevent your loved one from developing bedsores if you are not their primary caregiver. Yet, if you understand the actions that nursing assistants and other caregivers must take to prevent bedsores, you can advocate for your loved one and make sure they are getting the care they deserve.
Johns Hopkins, one of the United States’ most respected medical schools and facilities, recommends the following to prevent bedsores:
- Turn and reposition a bedridden person every two hours.
- Reposition those in wheelchairs every 15 minutes and ensure they sit up straight.
- Pad areas in a bed and wheelchair where pressure sores can occur.
- Ensure skin is always clean and dry so sores are less likely to develop.
- Ensure proper food and water intake to help bedsores heal when they do occur.
Long-term Medical Complications Associated With Bedsores
Nursing home residents who have little or poor mobility, those who are bedridden, and those who are in comas or a permanent vegetative state have the highest chances of developing bedsores. Stage I and II bedsores can be treated easily and often heal completely; however, the story changes when bedsores develop beyond stage II.
Residents who develop higher stage bedsores sometimes must deal with them for weeks or months before they heal. This is especially true for those who suffer from underlying health conditions such as diabetes. Some bedsores are so severe, medical professionals cannot categorize them. These “unstageable” ulcers can be fatal.
Examples of long-term medical complications associated with bedsores include:
- Infections. Once a pressure sore reaches Stage II, it is an open wound that can easily become infected. Infections in bedsores can enter the heart, bones, and bloodstream causing fevers, disorientation, an elevated heart rate, and general weakness. If left untreated, these infections can cause death.
- Amputation. Bedsores reduce or stop blood flow to affected areas. During treatment, doctors try to restore blood flow. Yet, some sores are too severe, forcing doctors to make the difficult choice to amputate a limb so they can save the person’s life. Amputation is not only a complication of severe bedsores, but it also can come with its own set of complications on top of the physical and emotional pain of losing a limb.
- Recurring Bedsores. The only way that bedsores can properly heal is with extensive bed rest. This can create a never-ending cycle of recurring bedsores when nursing assistants do not provide adequate care. Failure to turn and reposition residents can create new bedsores or cause existing bedsores to further develop.
- Autonomic dysreflexia. This is the medical term for the human body’s abnormal reaction to stimuli in the nervous system. Those who suffer spinal cord injuries and develop pressure sores have the most risk of experiencing autonomic dysreflexia. Some common symptoms include elevated blood pressure, muscle spasms, excessive perspiration, and paleness, redness, or bluish skin in the affected area.
The Financial Impact of Bedsores and Treatment
If you or a family member you love has developed bedsores as a result of caregiver neglect, you potentially face colossal expenses. The specific financial impact depends on the severity and number of bedsores and which course of action you take to deal with the neglect.
Examples of expenses associated with treating bedsores include:
- Medical expenses. You may know that developing bedsores means additional medical bills from doctor’s visits, medication, and sometimes hospitalization. Yet, you also may be faced with other medical expenses. Some who develop bedsores must undergo surgery, as well as costly imaging tests to examine the extent of the sores. Those who develop severe bedsores typically must also take prescription pain medication and antibiotics. When residents get stuck in a cycle of recurring bedsores or their sores aren’t healing quickly, these expenses can go on for months.
- Counseling. Many times the presence of bedsores on a resident of a long-term nursing care facility is an indication of a larger problem in the facility. A resident with bedsores may have suffered emotional distress because of the abuse and neglect they have suffered. Those residents who do not suffer from Alzheimer’s or dementia or aren’t in a coma or a permanent vegetative state may need to engage in therapy to work through their trauma. Depending on the extent of the neglect and abuse, some residents might need to utilize mental health services for the rest of their lives.
- Moving to another facility. If your loved one has developed bedsores because of intentional neglect or nursing home negligence, you may want to find them a new home. Change is traumatic for nursing home residents and it’s also inconvenient, and the financial consequences of transferring facilities can be overwhelming. Moving your loved one can mean paying much higher rates for a new nursing home or private nurse, or it can mean placing them in a facility much further away.
Four Steps to Take if Suspect Your Loved One Was Neglected
Florida law clearly defines abuse and neglect of the elderly and other vulnerable adults. Under Florida law, neglect is the failure to “provide an elderly person or disabled adult with the care, supervision, and services necessary to maintain the elderly person’s or disabled adult’s physical and mental health.”
Bedsores are a consequence of this failure. If you suspect neglect because of the presence of bedsores or other symptoms, you must stop the behavior as soon as possible.
You can take the following steps to start an investigation process and protect your loved one from further harm.
- Notify the administration. As soon as you notice bedsores on a loved one or if you have suffered bedsores from a neglectful caregiver, you must notify the facility’s administration. This can motivate caregivers and charge nurses to ensure your loved one’s bedsores receive the proper treatment and care.
- Notify DCF. Call the Florida Department of Children and Families (DCF) Abuse Hotline to report the neglect of your loved one. You can also file a report online. This will begin a formal investigation process through the state. DCF often shares information with other agencies and with a local prosecutor when they find evidence to support the complaint. The prosecutor will determine whether to criminally charge caregivers responsible for neglect.
- Notify AHCA. You can file a complaint about the facility by calling Florida’s Agency for Health Care Administration (AHCA) at (888)419-3456 or by submitting a complaint online. Once you file a complaint, it gets forwarded to an administrative unit that assigns the case. If the official who reviews the case believes residents are in immediate danger, they will inspect within two business days. Without immediate danger, the inspection can take longer. In either case, the AHCA will notify you of the outcome of the inspection.
- Contact a nursing home attorney. The law permits you to take action against caregivers who cause you or your loved ones harm through their abuse or neglect. Suing the facility and associated caregivers will not undo the pain of developing bedsores, but it can help cover the financial costs of treating them. Furthermore, a nursing home lawyer can help you complete the previous four steps, helping to ensure that other persons at the nursing home don’t suffer the same way your loved one did.
When Is a Nursing Home Liable for Neglect Due to Bedsores?
We discussed how painful and serious bedsores can be, and nursing homes can often prevent these injuries by providing adequate care for residents. However, nursing home residents suffer neglect far too often. When residents experience neglect from nursing home staff, many different injuries can occur – including bedsores.
If you believe that your loved one was the victim of neglect, resulting in painful and preventable bedsores or other injuries, you should not delay in speaking with a Fort Myers nursing home neglect lawyer.
Types of Nursing Home Neglect
Neglect involves omissions by nursing home staff that cause injury. Nursing home staff members should be well aware of the level of care each resident needs, and they should never fail to provide that level of care. When they do, residents can suffer unnecessary, costly, or even life-threatening injuries and medical complications.
The following are some common ways that nursing home staff members engage in neglect of residents. If you notice signs of neglect in your loved one, take action right away.
Mobility of Residents
As mentioned, many residents in nursing homes might be confined to a bed or a wheelchair for most of their waking hours. Nursing home staff needs to move residents around as much as they possibly can, instead of staying static in one place all day.
Failing to ensure that residents get shifted or moved regularly is a top cause of bedsores, as well as muscle and bone loss and other medical problems. Not being moved can also cause isolation, depression, and other mental injuries.
Improper Nutrition or Hydration
Nutrition refers to maintaining a balanced and healthy diet that provides your body with the proper nutrients. Nutrition is important for people of all ages, but older adults can have different nutritional needs. This is especially true for residents with certain medical conditions.
Staff members should be thoroughly familiar with the nutritional needs of each resident. For example, if one resident has diabetes or celiac disease, they will need a much different diet than others without those conditions.
Not receiving proper nutrition can lead to many issues:
- Weight loss
- Weight gain
- Hair loss
- Weakness
- Fatigue
- Disinterest in food
- Getting sick easier
- Longer recovery times
- Feeling cold
- Lack of concentration
- Medical complications
In addition to proper nutrition, staff members should ensure that residents all receive proper hydration. This is a particular concern for residents with cognitive or physical impairments, who might forget to drink water or might not get water for themselves when they want some. The sense of thirst can also decrease as someone ages, so staff must monitor and ensure proper water consumption. Signs of dehydration include confusion, dark urine, dizziness, fatigue, and more.
Unsanitary Conditions
Nursing home staff is in charge of keeping the facility – and the residents – clean. Some residents cannot physically bathe themselves or remember to do so, and staff members need to ensure they get properly washed regularly. In addition, clothing and bedding need to be cleaned regularly, especially if it gets soiled.
Unsanitary conditions are dangerous, as they increase the risk of serious infections. If a resident contracts an infection, it can result in stays in the hospital and other medical expenses, and infections can often be life-threatening.
Not Administering Medication
If a resident needs regular medication, it is often the staff’s responsibility to administer it. If staff members are not paying sufficient attention to their duties, they can make medication errors, including failing to distribute a dose or ensuring a resident takes their dose. Skipping doses of certain medications can result in serious medical complications.
Not Responding to Emergencies or New Medical Conditions
There is always the chance that nursing home residents will experience medical problems or emergencies. Residents might not always be aware of their symptoms, and staff should be aware of any new symptoms that residents might show that could indicate a medical problem.
In an emergency, the medical staff at a nursing home should react and provide treatment. This includes diagnosing the condition and ensuring the resident gets proper care, which could include transportation to a hospital. If staff members do not respond quickly to an emergency, it could constitute serious neglect that leads to severe medical injuries or death.
This form of neglect often applies to bedsores, as well. Once staff members notice that a bedsore is forming on a resident, they should address the matter right away. Timely treatment of bedsores can prevent the sores from worsening, if not resolve the problem completely.
On the other hand, when staff members fail to order necessary medical treatment of bedsores, the sores can unnecessarily worsen—and quickly. This constitutes neglect because the injuries would not be as bad or painful if staff members took the proper action for medical treatment.
Negligence of Nursing Homes
Neglect of staff members is only one of many causes of injuries to nursing home residents. In some situations, the problem stems initially from the negligence of the facility itself, and not necessarily of particular staff members. Nursing homes and parent companies can be negligent in a variety of ways, and these facilities should be liable for injuries to residents that result.
Negligent Hiring
As nursing populations grow across the United States, so does the number of staff members needed to provide care for residents. Turnover can also be high among nursing home staff, and this can lead facilities to rush to hire new people. Sometimes, nursing homes might not properly vet applicants and might hire people who should not be working in these facilities.
Some positions in nursing homes require a higher skill or education level than others. When hiring, a nursing home should make sure the person hired is qualified for the specific position they will hold. If someone is unqualified or too inexperienced, it can result in substandard care of residents.
In addition, nursing homes should conduct thorough background checks on all applicants they are considering. Facilities should never hire anyone with a history of domestic abuse or violence against others. Hiring people with prior criminal conduct against other people increases the chances that the staff member might engage in nursing home abuse.
Negligent Supervision
Once someone holds a position at a nursing home, they should abide by the required standard of care. If a nursing home fails to supervise staff members, they might engage in neglect or even abuse unchecked. This can breed a culture in which unnecessary harm to residents is common and allowed.
If a nursing home suspects – or knows – that a staff member engaged in misconduct that causes harm, the facility management should take disciplinary action right away. Nursing homes should never tolerate any form of neglect or abuse, and they should have policies in place to discipline or terminate staff who fail to provide the necessary standard of care. When nursing homes allow staff members to engage in misconduct unchecked, it opens the door for further harm to residents.
Violating Regulations
Each state has its own regulations for nursing homes, and facilities should always follow regulations.
These regulations are in place to ensure the health, safety, and well-being of residents, and some requirements include:
- Standards for cleanliness and sanitation
- The availability of medical treatment
- Proper security measures
- Food safety
- Hiring qualifications or disqualifications
When nursing homes violate regulations, there can be a higher risk of unnecessary and preventable injuries to residents, including bedsores.
While you might know that your loved one suffered unnecessary bedsores or other injuries, you might not pinpoint the source of the injuries or the responsible party. This is where an experienced nursing home neglect lawyer comes in. We can help identify the specific cause of your loved one’s injuries so we can prove a neglect or abuse claim against the facility.
Claims Against Nursing Homes
Identifying that your loved one has the right to file a claim is only the first step of the process. There are different types of injury claims depending on the specific legal principles at issue in your loved one’s case. The following are types of claims that might arise from serious and untreated bedsores.
Personal Injury
Personal injury is kind of a catch-all for legal claims arising from preventable injuries. In a personal injury claim, you assert that the nursing home – or individual staff members – were negligent, which resulted in the injury to your loved one.
To prevail in this type of claim, your loved one must demonstrate:
- The nursing home had the duty to abide by a particular standard of care
- The nursing home breached that duty
- The sub-standard care led to bedsores or increased severity of bedsores
- Your loved one suffered losses, including financial losses or pain and suffering, because of the bedsores
If an individual staff member was negligent, the nursing home can also be liable for negligence. This is because the law holds employers liable for the negligence of employees that causes injuries to others.
Medical Malpractice
One specific type of personal injury claim is for medical malpractice. Medical professionals should always abide by the standard of care set for their specialty, and this includes medical providers at nursing homes. Specifically, a medical professional should treat bedsores like another reasonably competent doctor would under similar circumstances. This includes treatment in the nursing home, as well as admitting the patient to the hospital if needed for serious bedsores or infections.
If a doctor or nurse at a nursing home does not provide proper bedsore prevention or treatment for existing bedsores, it can result in the unnecessary worsening of the resident’s condition. The resident can bring a medical malpractice claim against the medical professionals in charge of their care who did not adequately address the bedsore.
Nursing Home Neglect or Abuse
Another specific type of personal injury claim asserts neglect or abuse of nursing home residents by staff members. Neglect can rise above mere negligence, as staff members might know about bedsores and knowingly ignore the problem. Failing to report bedsores or make sure a resident gets treatment for bedsores can constitute neglect.
In addition, some nursing home staff members engage in the intentional abuse of residents. In this situation, a staff member might purposely leave a resident isolated and in one place for extended periods, which leads to bedsores and other injuries. If the cause of bedsores was intentional abuse, injured residents might recover punitive damages in addition to recovery for their other losses.
Wrongful Death
In drastic cases, bedsores can lead to life-threatening infections and other complications, which can lead to a resident’s untimely death. If you learn that your family member died, and the cause of death stemmed from untreated bedsores, you and other close family members may file a wrongful death.
Wrongful death cases claim that a death stemmed from the negligence, default, or wrongful act of another party. If a nursing home failed to treat bedsores with fatal results, it is likely the basis for a wrongful death claim.
In Florida, only certain family members can file this type of case, including:
- Spouse
- Children (including adult children)
- Parents
- Other relatives dependent on the deceased person
In nursing home bedsore cases, the claim often involves children and/or a spouse.
These family members and the deceased person’s estate can seek damages for:
- Loss of love and companionship
- Medical expenses before the death
- Burial and funeral expenses
- Lost inheritance
Speak with an experienced Florida wrongful death lawyer right away if your loved one passes away due to complications from bedsores while living in a nursing home.
Overall, bedsores can be a more serious issue than you might imagine, and improper treatment can lead to complications and even death. Always explore your or your loved one’s legal rights. Contact Viles & Beckman, LLC today for a free initial consultation.

 Click To Contact
Click To Contact