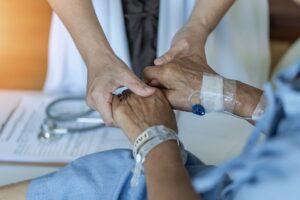
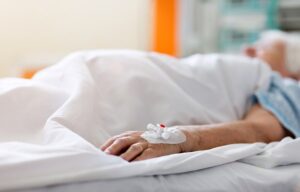
A recent study revealed that the mortality rate from falls experienced by people over the age of 75 more than doubled during a recent six year period. During that time, the death rate from falls in that age group increased from 52 per 100,000 people to 111 per 100,000 people. The health scientist at the Centers for Disease Control and Prevention (CDC) stated that the increase is most likely related to people living longer with conditions that, in the past, would have resulted in death. Additionally, the medications used to treat those conditions also contribute to an increase in falls.
Slips and falls are a major hazard for the elderly population. For assistance making sure your bills are covered, you need an aggressive and compassionate slip and fall attorney in Fort Myers to take your case. Read on for more information about the dangers of these types of accidents, the responsibility that nursing facility staff has in preventing this type of accident, and other ways to avoid falls among the elderly.
The Dangers of Slips and Falls for the Elderly
According to statistics provided by the National Floor Safety Institute, 60 percent of the deaths caused by falls occur in people 75 years or older. Falls are the leading cause of accidental injury and death among individuals aged 85 and older, and the second leading cause of accidental injury and death in those who are between the ages of 65 and 84.
One-third of the over-65 demographic in the U.S. will fall every year, and for many of these individuals, it isn’t the first time. Each year, approximately 1.8 million people over the age of 65 are treated at the emergency department for injuries sustained in a fall. The incidence of falls increases with every decade of life.
For elderly people who survive a fall, injuries are not only common but often severe. Falls account for 87 percent of the bone fractures incurred by individuals over 65 and are the leading cause of spinal cord injuries and traumatic brain injuries in this age group, as well. One of the most serious fractures that an older adult can suffer due to a fall is a hip fracture. Those over the age of 85 are 10 to 15 times more likely to fracture a hip during a fall than those in their 60s.
Half of all elderly individuals who suffer a hip fracture can’t return home or live independently after the injury, and 40 percent of all nursing home admissions are because an elder can’t care for himself or herself properly after being injured by a fall. Once an elder has entered a nursing home, however, the risk of falling doesn’t subside.
Expect More, Receive More: Legal Support That Feels Like Family
Nursing Home Fall Dangers
Over 60 percent of nursing home residents will suffer a fall in any given year, with most of these falls occurring while the resident is attempting to get into or out of bed, into or out of a wheelchair, or using the restroom or showering.
Beyond increasing age, internal and external risk factors for falling at a nursing home include:
- A history of falls, particularly in recent months
- Dizziness
- Cognitive decline
- The use of medications, particularly when the elder has recently started a new medication. Sedatives, anti-anxiety drugs, and other types of medication that affect the central nervous system are the most common culprits of medication-caused falls.
- Incontinence or urgency with toileting
- The elder exhibits agitation, confusion, or depression
- The elder requires oxygen or catheterization, both of which produce “tethers” that can cause the elder to trip or become entangled
- Diminished strength. Muscle weakness or walking or gait issues are the leading cause of falls in nursing homes, accounting for nearly one-quarter of all nursing home falls.
- Diminished sensation, vision, or hearing
- The facility has wet or cluttered floors or hallways. Environmental hazards, such as wet or cluttered floors, account for between 16 and 27 percent of falls.
- The floor surface has been freshly polished.
- The elder’s shoes do not provide adequate tread to prevent slips or are not properly fitted.
- The distance to the bathroom, the height of the toilet, and the presence (or lack) of grip bars in the toilet area
- Delayed staff response to resident’s call lights
- Poor lighting
- Incorrect bed height
The Responsibility of Fall Prevention in Nursing Homes
State and federal laws require that nursing homes certified by the Center for Medicare/Medicaid Services perform an initial assessment, as well as frequent updates to that assessment, on all residents entering the facility. Part of that assessment involves considering whether the resident is at high risk of falls and, if so, developing a fall prevention strategy.
Some of the considerations made when performing these assessments include:
- Is the room placement appropriate for this resident, or should the resident’s room be closer to the bathroom or the nurse’s station to meet his or her fall prevention needs?
- Does the resident need eyeglasses, hearing aids, gait belts, or assistive devices meant to reduce the risk of falling, and are these needs posted in the resident’s room for all staff?
- Will the use of vitamin D or calcium supplements better protect the elder from falls and fractures caused by falls?
- Does the resident’s family understand his or her risk of falling and their role in prevention?
- Does the resident have a high fracture risk that necessitates the use of hip protectors?
- Would the resident benefit from physical therapy to develop strength and prevent falls?
Nursing home facilities are also required to address fall prevention in their overall facility policies and protocols, which are made available for review by residents and their representatives, as well as state surveyors who conduct annual inspections as part of the Medicare/Medicaid certification.
Some considerations that regulators make when developing these policies and protocols include:
- How resident information is communicated between shifts, and how staff members are to address fall prevention strategies related to toileting, showering, and getting the resident to the dining area for meals.
- What measures should be taken to improve the environment and reduce the risk of falls? For example, should a facility install handrails so that all residents can move throughout the facility more safely? Should the nurses’ station be decentralized or the rooms redesigned to better assist those at higher risk of falling?
- Can psychotropic drugs that commonly result in falls be prescribed only as a last resort?
Medicare has raised the stakes for certified nursing homes, providing public access to health inspection reports and a rating system based on how many emergency department visits were made during the year due to residents falling at the facility. These ratings impact nursing homes’ bottom lines, as lower-rated facilities will be less likely to attract new residents.
Additionally, nursing homes found to have failed to provide appropriate fall prevention for a resident known to be at risk of falls can receive a deficiency on their annual inspection and may even be subject to financial penalties for failing to follow a resident’s assessment or failing to provide the resident with a safe environment.
Fall Prevention Tips for Caregivers
Around 77 percent of falls experienced by the elderly occur in the elderly individual’s home. While conventional wisdom says that having an elderly person who is at risk of falling remain seated when at all possible is the best way to prevent falls, it’s actually not true. Indeed, less activity causes increased weakness and results in more falls.
Elderly people need exercise to maintain their strength, with a suggested duration of 20 minutes a day of a combination of aerobic and anaerobic exercise. The Chinese martial art of tai chi can improve balance when engaged in by adults over the age of 70 at least twice a week for an hour. A study on tai chi and fall prevention found that an individual in this age group can reduce his or her risk of falls by 58 percent by engaging in regular tai chi practice.
Besides exercise, if you are providing care to an elderly person at home, adhere to the following tips to reduce the risk of falling:
- Carefully consider the safety of your flooring. Falls are more likely to occur if the elder’s home has loose or worn tile or uneven floors. AARP suggests installing carpet with a short, dense pile. Pay attention to any thresholds between rooms of the home with the understanding that just a fraction of an inch of rise between rooms can result in a trip.
- Attention should also be given to the lighting in the home, ensuring that light switches are easily within the elder’s reach and that stairs and other hazardous areas are well lit. Nightlights help provide some light if an elder cannot find a light switch.
- Promptly wipe up spills on hard surfaces to avoid slipping hazards. Think twice about applying floor wax to your tile floors or polish to wooden floors, as both of these can make the floor slick.
- You should have rubber bath mats in the tub or shower to help the elder avoid slipping while bathing, and the shower area should also have at least two grip bars. Toilet seats should be raised, and the toilet area should also have a grip bar.
- Ensure that the elder has an up-to-date eyeglass prescription and has had a recent hearing test. Losing one’s vision or hearing can prevent an individual from seeing objects that may cause a fall to take place or from hearing important instructions, such as “watch your step” or “the floor is wet.” If the elder wears bifocals, be aware that this type of eyewear can cause changes in-depth perception when the wearer is stepping onto or off of a curb. Only single-focus lenses should be worn outside.
- Use extra caution if the elder has recently started a new medication, as falls are most common within the first three days after the medication has been started. Remember that medications that assist the individual with sleeping are often associated with dizziness, which is a major cause of falls.
- Pay attention to the elder’s footwear. Slippers are comfortable, but they often do not provide adequate protection. Anything that allows the foot to move around will also increase the likelihood of a fall, as will high heels. Shoes should feature a flat sole, good tread, and be snug on the feet.
- Ensure that if the elder’s physician has recommended the use of a walker or cane, the elder has been trained to use it properly and is using it as directed.
- Provide chairs with stable armrests that the elder can use when standing up or sitting down.
- Eliminate clutter in the home. This means relocating or getting rid of not only boxes or stacks of items, but also removing small rugs and eliminating cords that are stretched across the floor. You should arrange furniture so that there is clear access between important areas of the home. Pets are another common tripping hazard, and you should vigilantly supervise your pet when in the presence of an elderly individual.
- Keep the elder hydrated, as dehydration is a common cause of dizziness. Bear in mind, however, that frequent hydration leads to frequent trips to the restroom. Pay attention to how far the senior needs to travel between the restroom and bed or a favorite chair, and how clear the path is between those locations.
You should also pay attention to any dizziness that the elder experiences. Whether on a new medication or not, discuss dizziness with a doctor, as well as unusual changes in behavior that may result from declines in the elder’s ability to hear or see.
If you or your loved one has been injured in a fall at a nursing home, explore the legal options available for obtaining compensation for damages caused by the accident by contacting a nursing home lawyer for a case evaluation.
Call or text (239) 334-3933 or complete a Free Case Evaluation form